The Shifting Baseline (part 2)
On March 1st, 1947, Eugene Le Bar, a 47-year-old American businessman, arrived in New York City by bus from Mexico City and nearly caused a medical disaster in the process.
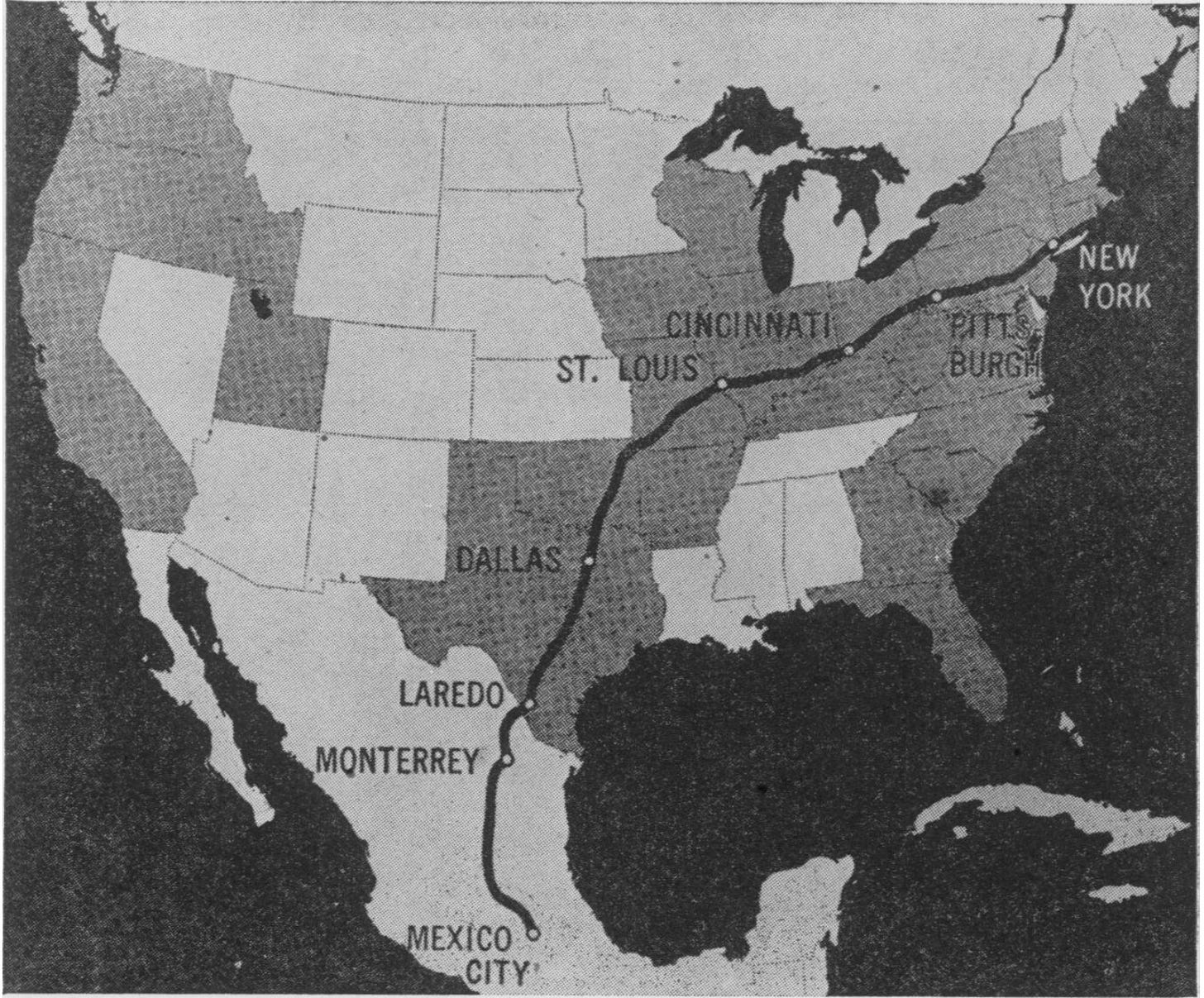
Le Bar’s trip from Mexico City to New York City (1947) P/C Life Magazine
He had a severe headache that aspirin wouldn’t touch, then developed a high fever and a strange, distinctive rash. Le Bar felt bad enough to be admitted to Bellevue Hospital on March 5. Because he had a smallpox vaccination mark on his arm, smallpox was initially ruled out. But on March 10th, Le Bar passed away after ten days of symptoms at Willard Parker Hospital for Communicable Diseases and after an intensive search for the diagnosis. [Weinstein]
Soon after, other people at Willard Parker Hospital began displaying similar symptoms. A 22-month-old baby named Patricia, a 27-year-old man from Harlem named Ismael Acosta, a worker at Bellvue Hospital who had contact with Le Bar, and a 30-month-old toddler named John all developed rashes that puzzled doctors. A positive diagnosis of smallpox was made on April 4, almost a full month after Le Bar first walked into the hospital with a headache, fever, and rash.
Smallpox vaccinations in New York City (1939)
Realizing that much of the city’s population was not adequately vaccinated against smallpox, later that afternoon, Israel Weinstein, the New York City Health Commissioner, held a press conference urging all New Yorkers who hadn't been vaccinated since childhood to receive another vaccination. The city quickly established free vaccine clinics and provided doses to private physicians.
The situation escalated on April 13 when a second person died from the disease. Mayor William O'Dwyer called for all 7.8 million New York residents to get vaccinated and publicly received the vaccine himself to set an example. The city mobilized its police, fire, and health departments, along with hospitals, to provide additional space for the vaccination effort. Doses of vaccines available on-hand were wildly insufficient for the entire city, but by scrounging vaccines from other states and the military, rapid response vaccine clinics were set up in all police stations and public health facilities.
By April 15, their epidemiological investigation showed that all diagnosed cases were closely related, and the outbreak had likely been halted through "ring vaccination"— tracing the movements of patients and vaccinating anyone who had contact with them until all possible contacts in the ring of connections had been vaccinated.
The response was remarkably swift and effective. In less than a month, over 6.3 million people were vaccinated. This massive effort is still considered one of the largest and most successful vaccination campaigns in history.
The 1947 smallpox outbreak in New York City serves as an example of effective public health response, demonstrating the importance of rapid action, clear communication, and public cooperation in the face of a health crisis. It also highlights the critical role of vaccines in controlling infectious diseases and offers valuable lessons for modern-day public health challenges.
In the aftermath of the outbreak, New York City and other jurisdictions reassessed their public health policies regarding vaccination and disease surveillance. The event highlighted the necessity for robust emergency response plans, including the need for stockpiling vaccines and establishing rapid distribution networks. The city’s health department had a real policy shift, and began to prioritize preparedness for future outbreaks, leading to improvements in disease tracking and response strategies.
The smallpox outbreak also spurred legislative changes at the state and federal level, including the reinforcement of vaccination requirements for school children. Prior to the outbreak, New York was one of only a few states that mandated vaccinations in schools, and even so, the smallpox vaccination level was inadequate to the threat. The crisis underscored the importance of vaccination as a public health measure, leading to broader acceptance and implementation of mandatory vaccination policies.
Because so many people knew and feared smallpox, these changes to require vaccines were widely accepted. The vaccination mandate extended to other common childhood diseases as well—measles, diphtheria, smallpox, whopping cough, scarlet fever, rubella—all of which were widely known and feared by earlier generations. 1
But after the introduction of effective vaccination programs, these diseases became so rare that the culture as a whole had generational amnesia and simply forgot about the terrible effects of the diseases. It only took a few more years for vaccinations to be called into question as problematic in and of themselves.
It's clear the generational amnesia can undermine the law’s ability to protect society at large. Vaccination laws and requirements capture insights that transcend generational forgetting. This syndrome arises when a legal program, like a school vaccination mandate, so successfully eliminates a societal problem, that citizens, politicians, and lawmakers forget that the program is in fact still working to keep that problem at bay.
This generational amnesia, in turn, can lead to changes in law and policy that undoes the earlier work, allowing the earlier problem to re-emerge. After the vaccines are forgotten, more children get diphtheria or whopping cough and die.
More recently COVID-19 vaccination mandates have become almost uniquely politicized. While COVID-19 is too new to suffer from the shifting baseline syndrome, decisions are being made will give the regulatory shifting baseline syndrome more room to operate, undermining the public health gains made by making vaccine-preventable diseases much in the United States.
Until the late 20th century, for most people the risk of various dread diseases was sufficiently high that they embraced new vaccines. The intentional result of federal and state vaccination regulations was that fewer people got these diseases. The perverse consequence was that as perceptions of disease risk changed with forgetting, getting the vaccines in your arm seemed like a far riskier option to many people. Consequently, pressures to eliminate or mitigate vaccination mandates increased. Perhaps most importantly, in the early 21st century, state legislatures increasingly enacted exemptions from school vaccination requirements, setting the stage for measles resurgences in 2015 and 2019.
For example, the measles vaccine was created in 1954, becoming increasingly effective and distributed widely in the 1960s. Following the introduction of the vaccine, many countries began implementing mass vaccination. The World Health Organization (WHO) established the Expanded Programme on Immunization in 1974, specifically targeting measles. [WHO] These vaccination efforts dramatically reduced measles cases worldwide. It was such a success that by the year 2000, measles was declared eliminated in the United States.
However, in 1998 a fraudulent study published in medical journal The Lancet falsely linked the MMR (the vaccine that protects from measles, mumps, and rubella) vaccine to autism. Unfortunately, this led to widespread public fear and misinformation, leading to decreased vaccination rates in some regions of the US.
Then, under public pressure government bodies started granting many different kinds of vaccination exemptions. Predictably, outbreaks of measles (and other preventable diseases) began again.
As vaccination rates fell below the threshold needed for herd immunity (approximately 95%), outbreaks began springing up in the U.S. and other countries. The resurgence of measles cases shows the challenges of maintaining high vaccination coverage amid vaccine hesitancy and misinformation, bringing up the even larger problem of keeping alive the knowledge of those dread diseases and how to use vaccines to eliminate them.
In this case, smallpox vaccinations stopped in the US after the disease was considered eradicated from the planet, and after massive WHO program to track down and vaccinate every last person on earth. That last person with naturally acquired smallpox was three-year-old Rahima Banu in Bangladesh. She was isolated at home with house guards posted 24 hours a day until she was no longer infectious. Remarkably, she survived, and with ring vaccination and isolation, no more cases were reported. With Rahima, last known case of smallpox in the wild disappeared from the Earth. [CDC2]
But measles is different; smallpox is gone, but there are a huge number of natural reservoirs of measles, so the threat of recurrence is high. Like Eugene La Bar’s case of smallpox, people can still move around the globe bringing measles with them. For such recurring threats, generational amnesia can be fatal. This is why laws requiring vaccination can capture a kind of medical wisdom that is able to transcend the years and the natural forgetting that takes place.
These days, getting a smallpox vaccination is no longer a part of childhood, it’s been taken out of the required vaccination set, a requirement that protects everyone, even if you’ve never known anyone who has had measles, mumps, rubella, diphtheria, tetanus, polio, or pertussis.2
Widespread vaccination policies are a way of getting around generational amnesia, and a way to help us all avoid the perverse and unanticipated consequences of forgetting.
____________________
[CDC] CDC Vaccine Basics
[CDC2] CDC History of Smallpox
[Conis] Conis, Elena. "Measles and the modern history of vaccination." Public Health Reports 134.2 (2019): 118-125.
[Craig] Craig, Robin Kundis. "The Regulatory Shifting Baseline Syndrome: Vaccines, Generational Amnesia, and the Shifting Perception of Risk in Public Law Regimes." Yale Journal of Health Policy, Law, and Ethics, 21 (2022): 1.
[Weinstein] Weinstein, Israel. "An outbreak of smallpox in New York City." American Journal of Public Health and the Nation’s Health 37.11 (1947): 1376-1384.
[WHO] WHO History of vaccination
In 1920, just 17 years earlier, there were around 110,000 cases of smallpox in the US. The chances were pretty good that you might have known someone with the disease
However, Diphtheria, Tetanus, and Pertussis (DTaP, DTP, Tdap, or Td): along with 5 doses of Polio (OPV or IPV); 4 doses for Hepatitis B: 3 doses or the Measles, Mumps, and Rubella vaccine (MMR): 2 doses Varicella (Chickenpox).